Jaw pain often starts small. You feel a click while chewing lunch in Bellaire, a tight pull near your ear during the drive through Houston traffic, or a headache that seems to settle into your temples by the end of the day.
Then it stops feeling small. Coffee gets harder to sip. Yawning becomes uncomfortable. Smiling for photos feels strained. If that sounds familiar, finding the right houston tmj specialist matters because jaw pain rarely stays neatly in the jaw. It can affect sleep, eating, speaking, and even how your teeth come together.
For many patients in Bellaire, West University, and nearby Houston neighborhoods, TMJ concerns overlap with other dental needs. Teeth grinding may wear down enamel. Bite strain may complicate cosmetic plans such as veneers or ClearCorrect. Poor nighttime jaw posture may also connect with snoring or sleep-disordered breathing. That’s why patients often do better with one dental office that can evaluate function, comfort, and smile goals together.
Facing Jaw Pain in Houston
A lot of people wait longer than they should.
They assume the pain is stress, sinus pressure, ear trouble, or just one of those things that will pass. But when your jaw hurts every morning, or your mouth opens with a catch instead of a smooth glide, your body is asking for a closer look.
Everyday moments that become frustrating
A patient might wake up in West University with tightness along the cheeks and temples, then notice lunch takes extra effort because chewing on one side feels easier than the other.
Another person might be sitting through a meeting near The Galleria and realize a simple yawn causes a sharp jolt near the jaw joint. Parents sometimes notice it at the worst possible time, like trying to eat birthday cake with their child while the jaw feels stuck halfway open.
These problems can seem unrelated at first:
- Morning soreness that feels like you clenched all night
- Headaches by late afternoon that keep returning
- Clicking or popping when you chew or talk
- Jaw fatigue after a long conversation
- A bite that suddenly feels “off” even though nothing obvious changed
Why local access matters
TMJ discomfort can be surprisingly disruptive because the jaw never really gets a day off. You use it while eating, speaking, swallowing, yawning, and often while sleeping if you clench or grind.
That’s why patients searching for a dentist near me or a dentist in Bellaire, TX often need more than a routine exam. They need someone who can connect jaw mechanics, tooth wear, headaches, and sleep-related habits in one place.
Practical rule: If jaw pain keeps returning, spreads to your temples or ears, or changes how you chew, it’s worth getting evaluated instead of trying to “push through” it.
When a practice can coordinate TMJ care with cosmetic dentistry, restorative dentistry, and sleep appliance therapy, treatment tends to feel simpler. You’re not bouncing between disconnected opinions. You’re getting one plan built around how your mouth functions day to day.
Understanding TMJ Disorders
The temporomandibular joint, or TMJ, is the hinge-and-glide joint that connects your lower jaw to your skull. You have one on each side.
A healthy TMJ works like a well-installed door hinge with a smooth track. It opens, closes, and slides with very little effort. When the hinge is strained or the movement becomes uneven, the whole system starts compensating.
Think of it like a misaligned door
If a door is hanging slightly crooked, it may still open. But it rubs, sticks, clicks, and wears down faster.
Your jaw can do something similar. If muscles pull unevenly, if you grind your teeth, or if your bite places extra pressure on one side, the joint and surrounding muscles may become irritated. Then simple motions start feeling harder than they should.
That irritation can involve different parts of the system:
- Muscle-related dysfunction often feels like tightness, fatigue, soreness, or tension headaches
- Joint-related dysfunction may involve clicking, catching, locking, or pain near the ear
- Mixed cases are common, where both muscle strain and joint mechanics play a role
Why stress and posture matter
Many people hear “TMJ” and think only of the joint itself. In reality, the muscles around the face, head, and neck matter just as much.
If you clench during stress, hold your shoulders high, lean forward at a computer, or sleep in a position that strains your jaw, those patterns can overload the system. That’s one reason TMJ symptoms often flare during busy work periods, poor sleep, or long hours at a desk.
Jaw pain doesn’t always mean something is badly damaged. Sometimes it means the joint and muscles are working too hard, too often, in the wrong pattern.
The role of teeth and bite pressure
Your teeth are part of the story because they guide how the jaw closes. If the bite is hitting unevenly, the muscles may adapt by pulling the jaw into a position that feels less stable.
That doesn’t mean every imperfect bite causes TMD. It means bite function can either calm the system down or keep irritating it. This is one reason some patients with worn teeth, cracked fillings, or shifting dental work notice more jaw strain over time.
For patients also thinking about cosmetic dentist near me, veneers, whitening, or restorative dentistry, jaw function should come first. A smile can look beautiful, but if the bite is unstable, cosmetic work may not feel comfortable or last as predictably as it should.
When normal fatigue becomes a disorder
A tired jaw after chewing gum all afternoon is one thing. Repeated pain, recurring headaches, and limited opening are different.
TMJ disorders usually move into “treatable problem” territory when you notice patterns like these:
- Symptoms keep returning instead of fading away
- Function changes, such as locking, catching, or limited opening
- Pain spreads into the temples, ears, face, or neck
- Teeth show wear from grinding or clenching
- Sleep and daily routine suffer because the jaw never feels relaxed
That’s where a careful dental evaluation can help. The goal isn’t to label every click as dangerous. The goal is to find out what structure or habit is driving the symptoms, then choose the least invasive way to settle things down.
Common Symptoms of TMJ Dysfunction
TMJ dysfunction doesn’t always announce itself clearly. Many patients first notice something indirect, like headaches, ear pressure, or sore teeth.
That’s why people often spend months treating the wrong problem.
Symptoms people often overlook
Jaw disorders can show up in ways that seem unrelated to the joint itself. You might feel discomfort near the ears and assume it’s congestion. You might wake up with temple pain and call it a migraine. You might notice a sensitive tooth and think you need a filling.
Common warning signs include:
- Clicking or popping sounds when opening or chewing
- A jaw that locks or catches for a moment
- Pain near the ear or along the cheeks
- Temple headaches that build during the day
- Facial muscle tightness when waking up
- Difficulty chewing tougher foods
- Tooth sensitivity or soreness from clenching pressure
- A bite that feels uneven or suddenly different
What these symptoms can feel like in real life
A busy professional may keep chasing headache relief without realizing the jaw is overworking all night.
A parent may blame ear fullness on allergies, when the nearby jaw joint and muscles are the source of the pressure. Another patient may notice they avoid crusty bread, steak, or wide bites because the jaw feels unreliable.
Those details matter. They help a clinician tell the difference between occasional tension and a pattern of dysfunction.
If your symptoms change with chewing, waking, stress, or jaw movement, the jaw itself may be part of the problem.
When to stop watching and get it checked
A single painless click isn’t always urgent. Persistent pain, repeated locking, or symptoms that interfere with meals, sleep, or daily comfort deserve more attention.
If you’re wondering how these issues can progress, this page on what happens if TMJ is left untreated gives a helpful overview of why ongoing symptoms shouldn’t be ignored.
Patients searching for an emergency dentist sometimes arrive because the pain has become sudden or intense. Even when it isn’t a classic dental emergency, it can still be important to evaluate promptly, especially if your mouth opening has changed or your jaw feels unstable.
TMJ Diagnosis with Tests and Imaging
TMJ diagnosis starts with listening, but it can’t stop there.
A useful exam connects symptoms with structure, muscle activity, bite force, and jaw movement. If someone only glances at your teeth and hands you a nightguard without a deeper workup, they may miss the underlying cause of the problem.
What a clinical exam can reveal
The first part of a TMJ evaluation is hands-on. A dentist checks how wide you can open, whether the jaw shifts to one side, which muscles feel tender, and whether the joints click or catch during movement.
They also look for clues inside the mouth:
- Flattened or worn teeth from grinding
- Cracks or stressed restorations
- Uneven bite contacts
- Signs that one side is taking more load than the other
This part matters because pain often comes from patterns, not from one isolated spot.
When imaging becomes important
Different imaging tools answer different questions. A standard dental x-ray may show broad issues, but some TMJ cases need more detail.
Here’s a simple comparison.
| Test | What It Reveals | Typical Use Case |
|---|---|---|
| Panoramic x-ray | General view of teeth, jawbones, and major structural changes | Initial screening when symptoms are broad or dental causes are also possible |
| CBCT scan | Detailed 3D view of bony structures and joint anatomy | Suspected structural joint issues, asymmetry, or bite-related planning |
| MRI | Soft tissue details, including disc position and joint inflammation patterns | Cases with locking, clicking, or suspected disc-related problems |
| Digital bite analysis | How force is distributed when teeth come together | Patients with uneven bite pressure, clenching patterns, or appliance planning |
| Muscle activity testing | How jaw muscles are firing and whether they are overworking | Muscle-dominant symptoms such as fatigue, tension, and clenching-related pain |
Digital analysis adds another layer
Some clinicians use advanced bite and facial measurements to understand whether the muscles and bite are working in harmony. According to Houston Dentists at Post Oak, physiologic dentists trained via LVI protocols can measure jaw muscle imbalances with 95% accuracy using computerized bite analysis and digital cephalograms.
That kind of data can be useful when symptoms are complicated, especially if the patient is also considering cosmetic dentistry or restorative work that could affect bite balance.
A good TMJ diagnosis answers two questions at the same time. What hurts, and why is that structure being overloaded?
Why precise diagnosis changes treatment
If the main issue is muscle tension, treatment may focus on reducing overload, calming clenching habits, and improving bite support. If the problem looks more structural, imaging may guide a different path.
That’s also why a general cleaning and exams visit isn’t always enough for jaw pain. Patients may come in thinking they need a filling, a tooth extraction, or dental x-rays for one sore area, then learn the discomfort is being referred from jaw muscles.
At Charles E. Boren, diagnostic tools such as digital x-ray imaging and bite-based evaluation can help sort out whether the problem is coming from tooth structure, joint mechanics, muscle strain, or a combination. That matters because the right diagnosis keeps treatment conservative whenever possible.
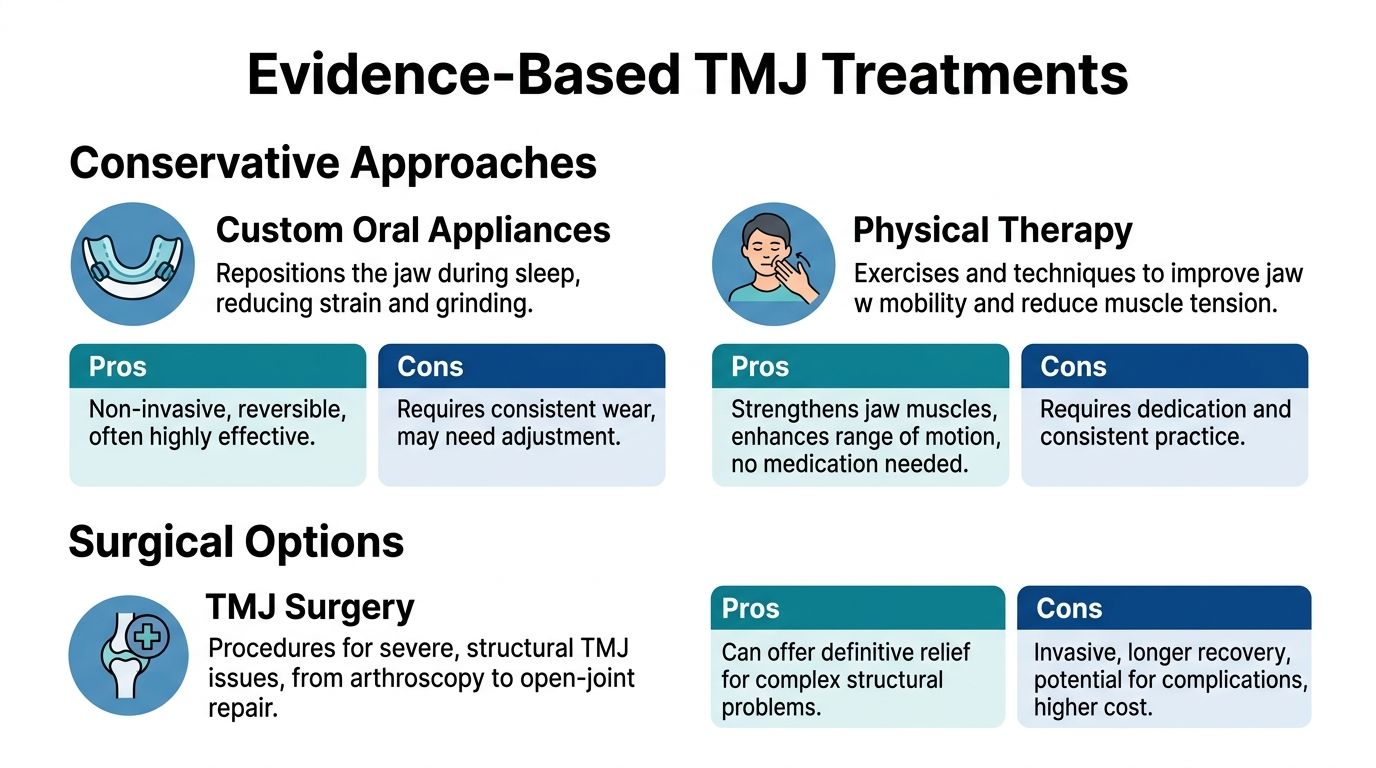
Evidence-Based TMJ Treatments
Most TMJ treatment starts with the least invasive option that fits the patient’s symptoms.
That approach makes sense because many people don’t need surgery. They need the joint unloaded, the muscles calmed, and the bite stabilized enough for the system to stop fighting itself.
Custom oral appliances
Custom oral appliances are one of the most common treatment tools. They fit over the teeth and are designed to reduce strain, guide the jaw into a more stable position, or protect the teeth from heavy clenching and grinding.
In the Greater Houston area, specialists have delivered over 8,000 custom oral appliances for TMJ and sleep-related breathing issues, according to Restore TMJ & Sleep Therapy. That volume tells you this approach is widely used in real clinical practice.
Pros and cons are fairly straightforward:
Pros
- Reversible care: Appliances can usually be adjusted without permanently changing the teeth
- Nighttime support: They often help patients who wake with soreness or grind in sleep
- Protection for dental work: Helpful for people with worn teeth, crowns, or cosmetic plans
Cons
- Consistency matters: You need to wear them as directed
- Adjustment period: Some patients need follow-up refinements before the fit feels right
If you want a focused overview of this option, this page on an oral appliance for TMJ explains how these devices are used.
Physical therapy and muscle-focused care
When the muscles are the main problem, physical therapy can be very useful. Gentle stretching, posture work, soft tissue techniques, and movement training can reduce the tension loop that keeps the jaw irritated.
Patients often do best when in-office care is paired with simple home routines. For a practical example, Joint Ventures Physical Therapy shares several TMJ pain relief exercises that show the kind of low-force movements many patients use between visits.
A few important points:
- This is active care: It works best when the patient practices regularly
- It supports function: The goal is smoother motion, not just temporary numbness
- It often pairs well with appliances: One reduces overload, the other improves movement patterns
NTI-tss and headache-focused options
Some patients have a strong headache or clenching component. In those cases, an NTI-tss device may be considered as part of a short-term or targeted strategy.
This small appliance is designed to reduce the intensity of certain clenching patterns. It isn’t right for everyone, but it can be a useful tool when the main complaint is muscle-driven headache pressure rather than joint locking.
Minimally invasive procedures and surgery
A smaller group of patients has structural joint problems that don’t respond enough to conservative care. Those cases may lead to procedures such as joint irrigation or surgical management.
This is usually reserved for situations where symptoms, imaging, and function all point in that direction. The point isn’t to rush there. It’s to use the right level of treatment for the actual problem.
This short video gives a useful visual overview of TMJ treatment thinking and how care can progress from conservative measures to more advanced intervention when needed.
How TMJ care can connect with cosmetic and sleep dentistry
Many patients find this surprising.
A worn-down bite may affect both comfort and appearance. A patient asking about teeth whitening or veneers may also need the jaw stabilized first. Someone searching for help with snoring may discover that a custom sleep appliance and TMJ therapy need to be coordinated so one goal doesn’t aggravate the other.
That’s why integrated planning matters. If one office can look at jaw strain, airway concerns, restorative dentistry, and cosmetic goals together, treatment tends to be more coherent and easier to follow.
Choosing Your Houston TMJ Specialist
Not every dentist treats TMJ problems the same way.
Some focus mainly on general dental care, which is fine for cleanings, new patient exams, and many everyday needs. TMJ cases are different because they often involve joints, muscles, bite dynamics, worn teeth, headache patterns, and sometimes sleep-related issues at the same time.
Credentials matter
The first thing to look for is advanced training. There are fewer than 300 board-certified Orofacial Pain dentists in the U.S., which underscores how uncommon this level of focused TMJ expertise is, as noted by Houston TMJ, Facial Pain & Sleep.
That doesn’t mean every good TMJ provider must hold that exact credential. It does mean you should ask direct questions about training, diagnostic method, and how the office handles complex jaw pain.
A practical checklist
When comparing providers, use a checklist instead of choosing based on proximity alone.
- Diagnostic depth: Do they evaluate bite, muscles, joint movement, and imaging when needed?
- Conservative mindset: Do they start with reversible options before talking about major procedures?
- Related services in one place: Can they coordinate TMJ care with sleep appliances, restorative dentistry, or cosmetic planning?
- Comfort support: Do they offer sedation options if dental anxiety makes treatment harder?
- Payment clarity: Can the team explain financing, phased care, and expected follow-up in plain language?
Communication counts more than people realize
TMJ treatment often unfolds over time. You may need appliance adjustments, symptom tracking, and coordination with another clinician.
That’s why communication systems matter. If you’re comparing healthcare offices in general, this overview of a HIPAA compliant communication platform gives useful background on why secure patient messaging and follow-up tools are worth asking about.
The right specialist doesn’t just name the problem. They explain what they found, what they’re ruling out, and what the first conservative step should be.
Why patients in Bellaire and nearby Houston often prefer integrated care
A patient may start by searching dentist near me because of jaw pain, then discover they also need help with a damaged filling, tooth wear, snoring, or a cosmetic concern caused by years of grinding.
That’s where a Bellaire practice can be especially helpful if it already offers broad dental care under one roof. Instead of treating TMJ in isolation, the office can connect it with bite protection, restorative planning, and long-term smile goals.
For patients near Bellaire, West University, and central Houston, convenience also matters. A calm office close to daily routines makes follow-up much easier, and TMJ care often depends on follow-up.
What to Expect at Your First TMJ Appointment
A first TMJ visit should feel organized, not rushed.
Most patients are relieved when the appointment is more like an investigation than a sales pitch. The goal is to understand your symptoms, how long they’ve been happening, what makes them worse, and what your mouth is doing mechanically.
The conversation comes first
Expect questions about when the pain started, whether it’s worse in the morning or evening, and whether chewing, stress, or sleep changes the pattern.
You may also be asked about:
- Headaches or migraines
- Clicking, locking, or limited opening
- Past dental work
- Grinding or clenching habits
- Snoring or poor sleep
- Neck and shoulder tension
These details help connect the dots. Jaw pain that’s worst on waking suggests something different from pain that starts only after a long meal.
The exam is usually more detailed than a routine checkup
A TMJ-focused dental visit often includes checking your bite, feeling the chewing muscles, listening for joint sounds, and measuring how your jaw opens and tracks.
If needed, the dentist may recommend dental x-rays or additional digital imaging to see whether the issue looks tooth-related, muscle-related, joint-related, or mixed. The point is precision. You don’t want to treat a muscle problem like a tooth problem or vice versa.
You should leave with a clear first step
A good first appointment usually ends with a simple, understandable plan. That may include an oral appliance, home care guidance, muscle relaxation strategies, or referral for additional imaging if the joint needs a closer look.
Patients also appreciate hearing what is not recommended yet. Sometimes the best plan is to avoid rushing into irreversible bite changes until the jaw has stabilized.
Here’s what many patients want clarified before they leave:
| Topic | Why It Matters |
|---|---|
| Working diagnosis | Helps you understand what structure seems to be driving symptoms |
| First treatment step | Keeps the plan manageable and conservative |
| Follow-up timing | TMJ care often needs adjustments based on response |
| Cost and financing | Lets you plan without surprises |
| Impact on other dental care | Important if you also need restorative or cosmetic treatment |
Questions worth asking
You don’t need to know dental terminology to ask good questions.
Try these:
- What do you think is causing my symptoms most directly?
- Are my muscles, joints, or bite the main issue?
- What conservative treatment would you start with first?
- Will this affect future cosmetic dentistry or restorative work?
- If I also need help with sleep breathing, can that be coordinated here?
That last question matters more than people realize. Some patients come in focused on jaw pain and later learn their nighttime clenching, snoring, and airway strain are part of the same larger picture.
Next Steps and Scheduling Your Consultation
If jaw pain has started shaping your meals, sleep, or workday, it’s time to stop guessing.
The right next step is a focused evaluation with a local dental office that can look at the jaw, bite, muscles, and related concerns together. For many adults in Bellaire, West University, and Houston, that means choosing one practice that can also help with ongoing dental care, restorative needs, cosmetic planning, and sleep appliance coordination when appropriate.
If you’ve been searching for a houston tmj specialist, a dentist in Bellaire, TX, or even an emergency dentist because the pain has become hard to ignore, early evaluation can make treatment simpler. It can also help prevent unnecessary dental work on teeth that may only be hurting because the jaw system is under strain.
The first visit doesn’t commit you to a major procedure. It gives you answers, a direction, and a practical first step.
If you're dealing with jaw pain, headaches, clenching, worn teeth, or related sleep concerns, schedule a consultation with Charles E. Boren in Bellaire. The practice serves patients from Bellaire, West University, and Houston with personalized dental care that can coordinate TMJ therapy, oral appliance treatment, cosmetic planning, and everyday dental needs in one setting.